As the world marks the 2026 World Neglected Tropical Diseases (NTDs) Day, Nigeria’s fight against the diseases faces mounting challenges that experts warn could derail progress toward the 2030 elimination targets.
Despite notable gains, including the eradication of Guinea worm and significant reductions in trachoma and lymphatic filariasis, donor withdrawals, insecurity, regulatory bottlenecks, and inadequate domestic funding now threaten to reverse years of progress.
Over 100 Million Nigerians at Risk
According to official data, 771 of Nigeria’s 774 local government areas are endemic for at least one neglected tropical disease, leaving more than 100 million Nigerians at risk. The World Health Organisation (WHO) estimates that Nigeria accounts for 25 per cent of the global NTD burden and about half of Africa’s total cases.
Of the 21 NTDs identified by WHO, 15 are endemic in Nigeria, with all 36 states and the Federal Capital Territory affected by at least one disease. Common NTDs in the country include lymphatic filariasis (elephantiasis), onchocerciasis (river blindness), schistosomiasis (bilharzia), soil-transmitted helminths, and trachoma.
Although Nigeria eliminated Guinea worm decades ago, yaws, once eradicated in 1945, has resurfaced.
Experts estimate that about N8.6 billion is required under the national master plan to effectively combat NTDs.
Medicine Bottlenecks and Import Restrictions
While many life-saving medicines for NTDs are donated free of charge by pharmaceutical companies, regulatory hurdles are disrupting access.
Drugs such as Mebendazole, Albendazole, and Praziquantel, essential for treating intestinal worms, are listed under the National Agency for Food and Drug Administration and Control (NAFDAC) Ceiling List, which restricts importation of medicines that can be produced locally.
The policy is designed to promote local manufacturing, but health officials warn that there is currently no budgetary provision to procure these medicines domestically, creating artificial shortages and threatening treatment campaigns.
The National Coordinator for NTDs at the Federal Ministry of Health and Social Welfare, Dr Fatai Oyediran, said the ministry is seeking a three-year moratorium to allow continued importation of donated medicines while efforts are made to integrate them into government budgets.
“These medicines are donated, not procured,” Oyediran explained. “We are not against local production, but we do not have funding to buy them locally. That gap is affecting implementation.”
He noted that Nigeria has removed over 30 million people from treatment programmes out of the initial 91 million treated nationwide, while about 39.5 million people have been cleared from lymphatic filariasis treatment lists. The country has also recorded an 84 per cent reduction in trachoma cases.
Donor Exits, Insecurity Compound Challenges
The withdrawal of key partners, including Research Triangle International following U.S. funding cuts, has added pressure to Nigeria’s NTD response.
Sightsavers Country Director, Prof. Joy Shu’aibu, said insecurity in some states has slowed field assessments and disrupted programme delivery. In Zamfara, for instance, assessments in 14 local government areas aimed at determining whether to stop long-term elephantiasis treatment have stalled for four years due to security concerns.
Similarly, assessments in Imo State were delayed for more than five years before completion in late 2025.
Shu’aibu noted that while mass drug administration campaigns remain largely effective and free to beneficiaries, insecurity, dwindling donor funding, and high attrition of health workers continue to hamper progress.
Nevertheless, she expressed optimism that Nigeria could eliminate river blindness, trachoma, bilharzia, intestinal worms, and elephantiasis by 2030 if current momentum is sustained.
Weak Primary Health Care Integration
Health experts argue that Nigeria’s heavy reliance on campaign-style mass drug administration is insufficient for long-term elimination.
Dr Sunday Udo, National Director of The Leprosy Mission Nigeria, emphasised the need for stronger integration of NTD services into routine Primary Health Care (PHC).
He explained that while preventive-chemotherapy NTDs benefit from mass treatment campaigns, case-managed diseases such as leprosy, Buruli ulcer, and snakebite require early diagnosis, consistent treatment, and long-term follow-up, areas that depend on functional routine healthcare systems.
“Insecurity, weak health system integration, and dependence on partner support make the programme fragile,” Udo said. “Elimination requires strong PHC systems, laboratory support, referral networks, and community health workers.”
He also warned that without improvements in water, sanitation, and hygiene (WASH), reinfection will continue, particularly for intestinal worms and schistosomiasis.
Call for Whole-of-Government Approach
Stakeholders are urging federal, state, and local governments to adopt a “whole-of-government, whole-of-society” strategy, increase predictable domestic financing, and create dedicated NTD budget lines.
They stress that tackling NTDs is central to achieving Sustainable Development Goal 3 and breaking the cycle of poverty, as the diseases disproportionately affect poor and underserved communities lacking safe water, sanitation, and adequate housing.
With more than 100 million Nigerians still vulnerable and 771 LGAs endemic, experts warn that without urgent action to fix medicine supply chains, boost funding, and strengthen primary healthcare integration, Nigeria risks missing its 2030 elimination targets, leaving millions exposed to preventable disability and poverty.
World NTD Day, observed annually on January 30 and recognised by the World Health Assembly in 2021, aims to mobilise global action, funding, and collaboration to control and ultimately eliminate these diseases. For Nigeria, the message this year is clear: progress is real, but it remains fragile.
Health
 News MasterUpdated 2 months Ago3 Mins read71 Views
News MasterUpdated 2 months Ago3 Mins read71 Views
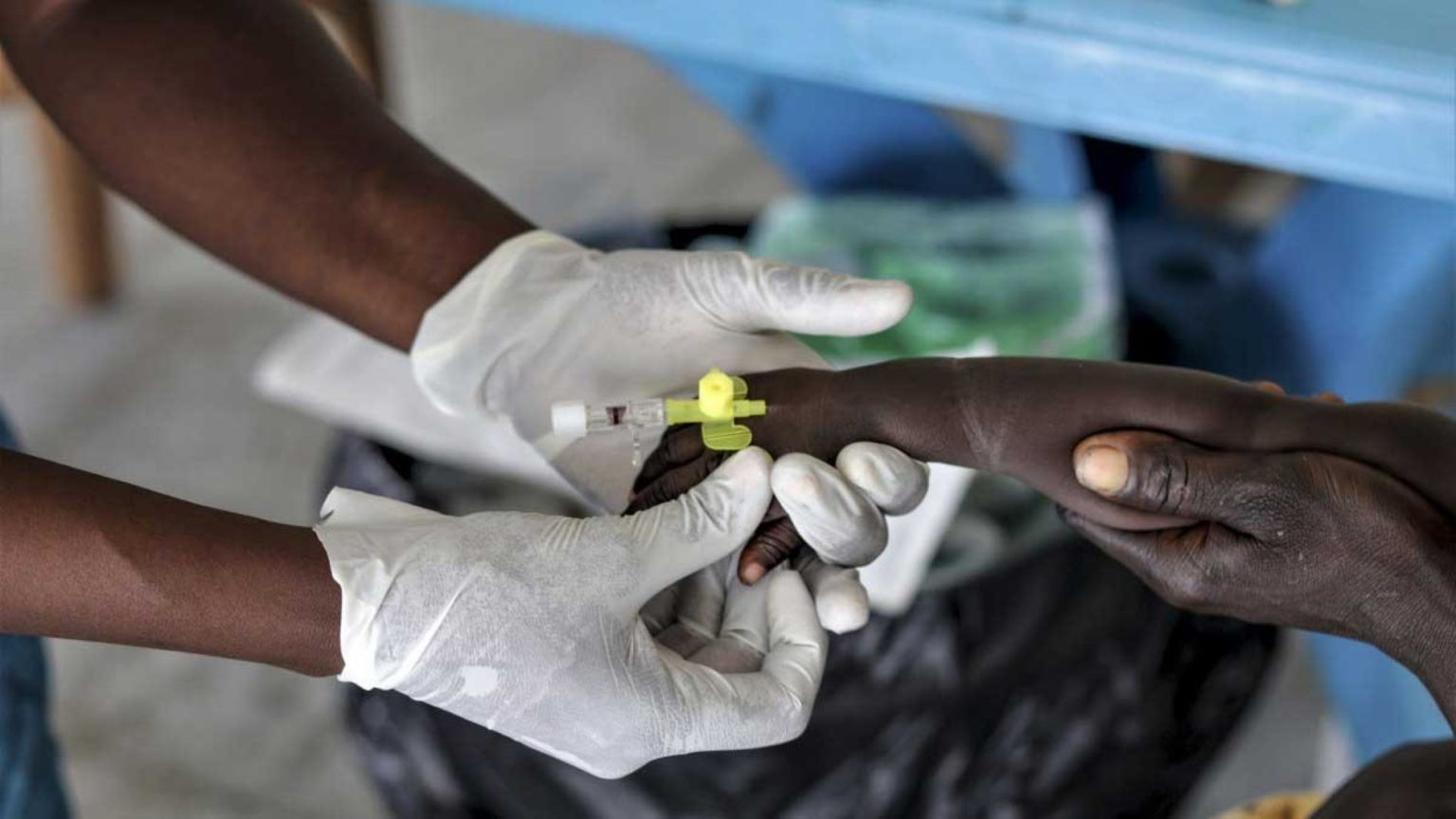
Drug Shortages, Funding Cuts Threaten Nigeria’s NTD Elimination Drive
Share
Latest Posts
Related Articles
Health
WHO Pushes for Faster Global Response as Hepatitis Elimination Goal Faces Delay Risks
The World Health Organization has raised concern over the slow pace of...
3 days Ago
Health
Lagos First Lady Supports Lifesaving Child Surgery with N70m Health Intervention
The wife of the Lagos State Governor, Dr. Ibijoke Sanwo-Olu, has strengthened...
4 days Ago
Health
FCT Begins Deployment of New Long-Acting HIV Prevention Injection
The Federal Capital Territory Administration (FCTA) has commenced the introduction of a...
4 days Ago
Health
Lagos Event Puts Spotlight on Women’s Health During IWD Commemoration
Health advocates and stakeholders gathered in Lagos to mark the 2026 International...
4 days Ago











Leave a comment